I find the field of eating disorders to be incredibly fascinating, challenging and rewarding. Becoming a nurse practitioner after practicing as a dietitian has only added to my interest. The physiology of the body is so interesting, especially when it comes to how the body is able to compensate in order to stay alive in the presence of starvation, purging and other physically taxing circumstances. That doesn’t mean the body is healthy and it’s functioning optimally and there aren’t very severe long term consequences, there are of course. But the fact that our bodies can withstand extreme conditions and still survive is amazing.

A lot of the things I’m going to talk about in this post I talk about with patients and clients. Unfortunately, doctors and nurses don’t get much education in eating disorders during their training even though eating disorders affect 1 in 20 women in the community (source). That’s quite common! I have a lot to learn, but from what I have learned over the past several years is that the medical complications that arise as a result of an eating disorder and disordered eating behaviors can be missed completely or misdiagnosed and mistreated. I have a lot more still to learn, but I think being able to understand the medical complications of eating disorders can be really empowering when helping a patient/client feel motivated to continue recovering and healing. Being able to explain the subtle and also more extreme ways in which your body is telling you that in fact, it’s not “fine” can give the healthy side of your brain some ammunition when it comes to fighting off the unhealthy side of your brain convincing you to continue in unhealthy behaviors.
What I hope this post does is bring clarity to your questions and confusion and also provide resources that you can bring to your health care provider so the both of you can partner together in your journey. I also hope this is a good starting point for you, but by no means is this post completely comprehensive because that would take a novel) There aren’t a lot of physicians and nurses adequately knowledgable when it comes to medically managing the complications that arise with an eating disorder. While I hope that changes, it makes sense given the lack of education. So what can be helpful if you don’t have a health care provider who is knowledgable, is to bring them resources and research articles so they can help you best.

LABS ARE NORMAL
If you are purely restricting your food intake, then we actually expect all the labs you get drawn at your doctors office to be normal. This is your body being really good at making sure you survive and compensating in an unfavorable environment. With that said, there are some people who do experience abnormal lab values (like electrolyte levels, your white blood count or hemoglobin and hematocrit levels among many others) and we don’t have an exact reason why. Some people’s bodies compensate better than others just like some people experience more gastrointestinal issues than others. The important thing to keep in mind is that just because you have normal labs doesn’t mean your body isn’t suffering. Often the only abnormal finding that objectively shows the patient their body is suffering is the DEXA scan showing low bone density. I heard Dr. Gaudiani share this analogy once that I thought was brilliant. It’s the house on fire analogy. If a firefighter comes to your house and you’re standing outside and he says, “hey ma’m, you’re house is on fire!” and you’re like, “no it’s not, I don’t see the fire and the sidewalk isn’t bubbling” they are going to get out all their equipment and put out the fire. Just because the sidewalk isn’t bubbling, doesn’t mean you don’t have a massive fire that is dangerous, life threatening and needs to be put out.
LOW THYROID HORMONE
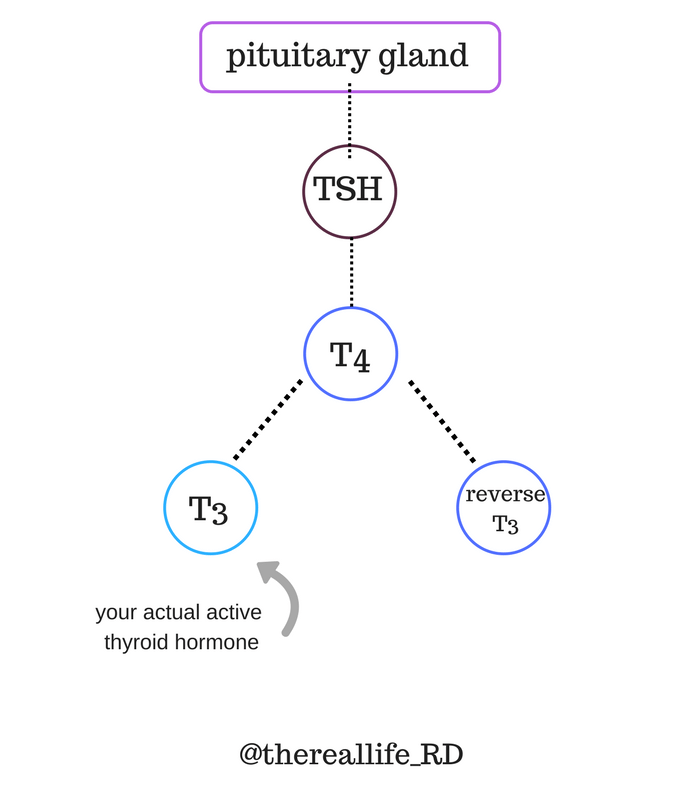
Whenever your body is under a severe amount of stress – from being critically ill, recovering from surgery or a trauma, restricting calories etc – the thyroid takes a hit. And when this happens you can see low thyroid levels show up on lab work. Since we’re talking about eating disorders and disordered eating here, this could be a finding in your lab work if you’ve been restricting calories and/or at a low body weight. Most commonly, you’ll see low T3 levels and low T4 levels, but normal TSH levels. In order to rule out a true hypothyroid disorder like Hashimoto’s your doctor would want to draw thyroid antibodies. If those are normal, medication is inappropriate and not indicated. Your thyroid levels will restore back within normal range as your body is nourished adequately and your weight is restored to a healthy place for your body.
ELEVATED LIVER ENZYMES
Your doctor may have told you that you had high liver enzymes on your blood work. These enzymes are abbreviated AST and ALT. There are varying levels of severity with this, but it’s possible for you to see higher than normal liver enzymes on your blood work as you recover from your eating disorder – especially if you’ve been restricting calories and starving yourself for some time. This happens because essentially your liver is starving and so your liver cells start dying. So these elevated enzymes show us that actually, your body isn’t fine and it needs nourishment and healing.
ELEVATED CHOLESTEROL LEVELS
I have clients currently and many patients who experience elevated cholesterol levels during their recovery from a restrictive eating disorder. I’ve also gotten this question in emails from readers. This can become a really tough mental game for patients/clients because it can cause them to think, “I need to change my eating and exercise to bring down my cholesterol!” If your health care provider isn’t aware of your history and/or knowledgable about eating disorder pathophysiology they might make a well intended suggestion to change your eating or exercise habits to lower cholesterol or refer you to a dietitian with that recommendation. Ahhhhhh. Well intended, but so unhelpful. High cholesterol levels are a way your body is compensating for the restriction – it’s the way your body alters cholesterol in order to attempt to keep you safe. So as you learn to normalize your eating and adequately nourish your body, your cholesterol will normalize with time.

AN “ATHLETIC HEART”
This isn’t a lab, but a vital sign and it’s more important than any of the above. Just because your heart rate is slow (<60 beats per minute) doesn’t necessarily mean you’re physically fit and therefore your heart is extra healthy. When you’re not feeding your body adequately, over time your muscles deteriorate and your heart is a muscle. So your low heart rate could actually be telling you how much your body is suffering and this is one way it’s compensating. Other ways (among other things) might be lower body temperature so you’re always cold, low blood pressure so you’re lightheaded, and low blood sugar leaving you lightheaded, shaky, and not able to think. To test if your low heart rate is because you have an athletic heart vs a starved heart your doctor can have you exert energy in some way. An easy way to do this is to walk about 10 feet, turn around and walk back. If your pulse increases (usually by 1.5x or 2x the rate it was when you were resting) then you do not have an athletic heart. If your heart was strong and healthy, it would hardly know the difference between resting and walking. A starved heart on the other hand has to work a lot harder when subjected to very mild exertion like walking a short distance.
I hope this was helpful if you are in recovery or if you have a loved one that is in recovery. And if you are a health care provider, dietitian or any other health professional, I hope this was informative as well and a stepping off point to continue learning and reading! I 100% believe that anyone can find complete healing whether you’ve been struggling with an eating disorder for decades or are struggling with yo-yo dieting and disordered eating and exercise patterns. Everyone deserves to get the support they need <3
Sources
Mehler, Philip S. and Andersen, Arnold E. Eating Disorders: A Guide to Medical Care and Complications. Baltimore: Johns Hopkins University Press, 2010. Print.
The Academy of Eating Disorders. Eating Disorders: A Guide to Medical Care. Retrieved from https://static1.squarespace.com/static/57028b61b654f934aedcedba/t/586d3c839de4bbad0ca3772b/1483553925826/AED+Medical+Care+Guidelines_English_12.15.16.pdf
Mehler, P.S. and Brown, C. (2015). Anorexia Nervosa: Medical Complications. Journal of Eating Disorders, 3(11). doi:10.1186/s40337-015-0040-810.1017/S0003055403000534
















Great!
In addition: low B12 and D vitamin, that can be contributing to tiredness and low bone density (that by low D vit of course).
Plus very relevant – electrolytes, especially K, as low levels of this can be extremely dangerous for the heart (see arrhythmias, sudden cardiac arrest).
You have addressed low hormone levels earlier, but this is also something they might draw bloods for.
Keep up the great work!
Merle (in training to become a physician :-))
Totally agree with you Merle! Of course this post isn’t comprehensive as we’d be writing 5000+ words but hopefully a jumping off point for people. Typically we see low K values in patients with purging behaviors vs purely restrictive
YASSS girl. Eating disorder RD here. This is so helpful- I have trouble sometimes communicating in real words what my patients’ labs mean. I want to print this out and keep it by my desk!
So glad it was helpful! Of course, there is a lot more to note here and dialogue through but hopefully this is a starting point. 🙂
I experienced all of that when recovering from anorexia including the clueless doctor. Medicaid had placed me with a naturopath who, at my first appointment, told me she had worked with a lot of people with eating disorders. She had me get some labs done and when she saw my high cholesterol she asked what I had been eating. I told her I had had peanut butter and crackers for lunch (which was a huge win for me, pb was a fear food at the time) and she shook her head. She told me that not everyone has high cholesterol when recovering if they are eating healthily. She then gave me a list of green smoothies. Luckily, I was also seeing a non-diet dietitian who specializes in eating disorders and is amazing. She had told me that the off labs are completely normal and should resolve on their own. I chose to believe her. If I hadn’t had that knowledgeable person in my corner, I easily could have nose-dived back into anorexia from my encounters with my doctor. I hope education around eating disorders for medical practitioners becomes more prevalent. So many people suffer and are triggered or go undiagnosed because of insufficient training.
Oh man Hillary thanks so much for sharing and I’m so glad you had a knowledgable RD who you trusted. <3
This is a phenomenal post! I’m definitely saving for later to refer back to. As an eating disorder therapist who doesn’t have as much nutritional/medical knowledge, this is extremely helpful for ME in working with my clients and understanding their medical records. I think it will also be helpful when coordinating with their treatment team.
Just another note… When I was working on my certification for treating eating disorders I was already on the path to recovery. But it wasn’t until I started learning and reading more about the physical consequences and medical indicators of starvation that I REALLY understood just how scary these disorders can be. I was surprised to learn I had suffered from so many of the indicators early on and, like you mentioned here, were missed or written off in my physical exams. Looking back at the whole picture, I now know just how scary things could have been.
Great work and thank you!
When I was first being treated for anorexia and obsessive exercise, a cardiologist told me that my low heart rate and lean body were just genetic and due to being an athlete. He told me there was no way I was eating as little as I reported and running as much as I was. He said it wasn’t possible. My eating disordered brain loved that comment So I left that appointment and went directly to the gym because the professional told me there was nothing wrong with me. So many doctors have no clue about EDs and are doing harm to those already suffering. I am incredibly grateful that I have an amazing PCP and worked with an ED therapist who were able to support me in my recovery.
Robyn, I found this post INCREDIBLY helpful, thank you so much!! One thing that I am currently struggling with in my recovery journey is how to deal with the anxiety that comes with a growing body size around naive family and friends? I don’t want to tell everyone my story but their judgement (or I guess what I perceive as their judgement) is killing me!! 🙁
WOW. I was blown away by what you said about cholesterol. About 3-4 years ago when I was still not having a period and still recovering I got a blood test done and had high cholesterol. Now I kind of wonder what it would be.
The “athletic heart” comment is SO important. When I was struggling with my ED way too many doctors assumed that my low heart rate was because it was strong from running. Only one nurse at a German hospital became concerned after checking my heart rate. I had all the other symptoms as well, low blood glucose, low bp, freezing, dizzy; I was essentially a walking cry for help and no one ever questioned me. To be honest during recovery I was a little angry that none of my doctors ever noticed what was wrong for years. But, now I am using that anger as a motivation to go back to school to become a health professional who will notice and help people get the help they deserve. Thank you for sharing this!
I’m so sorry for your experience Molly, but I’m so glad you’re channeling that into positive passion!
Thank you for this! Now i know why my liver has come back elevated and the doctors had no explanation for it. Makes me feel more comfortable knowing that it is due to restricting and now that I am headlong into recovery perhaps this might fix itself!
so glad it was helpful!
Dear Robyn,
Thank you, thank you, thank you!
I’ve had AN/BN for quite a long time. On a couple of different occasions, when I was still in high school, I’d been told by my GP that my cholesterol was slightly elevated (he knew about my health issues) and told me that I should change some of my food choices. He pulled out a peiece of paper and wrote down his reccomendations of things to avoid/ substitute.
My whole life, my family has been unhelpfully health conscious, and are always reminding me to “watch what you eat”… so finding this out brought me a huge sense of shame and self-disgust, beyond what I had already been feeling. I felt so much pain in thinking that I could be considered to be eating in excess/“unhealthily” when I was already underweight, restricting and exercising obsessively. I also felt so angry at my body, because I knew how much energy and effort had gone into being so strict around food, and yet it still wasn’t enough?!
I’m now 27 but that experience has stuck with me all these years. Shame is so damn relentless! Despite my emotional brains stubborness around it, it’s really nice to intellectually know that maybe it WAS my eating habits that contributed to such labs, but maybe not the kind of habits I had assumed had been the cause of it afterall…
Really wish we had more dietitians like you around in Sydney, Australia!
I wish I had read this before starting thyroid medication a year ago!!! My levels were ever-so-slightly sluggish, so my doctor prescribed me levothyroxine in hopes that it would also help regain my period. Now I’ve recovered, I feel like I’m stuck on it! Not only that, but they’ve slapped a pcos diagnosis on top of it, and I just feel so….misunderstood.
I’m struggling with this now. I’m just over two years inrto recovery and my weight has only just stabalisted. I’m 37 with a 10/15 year history of disordered eating. I recently went to the doctor to have my reproductive hormones checked and they did a liver panel which has shown that My ALT is slightly elovated. Everything else they tested is normal. I have tk go an have an ultrasound but I’m m panicing as if I have fat in nh liver I know they will just recomend weightloss. I can’t doet again. I gained 80lbs in recovery. I’ve sear he’d everywhere for information. All my results were normal before. I don’t know if it could still be my recovery causing it, this far in. I don’t know if I should listen to the doctors advice and diet or ignore it and continue with recovery. It’s really stressful. Hope someone has some advice or input. Thanks x
Hi! I’m 14 years old and I’m currently recovering from anorexia. Recently I went to a doctor check up and she was shocked that I lost so much weight (12 pounds) i didn’t tell her about my eating disorder because i was in fear that she might send me off to a hospital. she then asked for blood tests to be done and turns out i have some high liver levels or something like that and im FREAKING OUT. i have no idea if i did my recovery wrong because it’s only been 2 weeks! im also currently experiencing extreme hunger so i have no idea if i should just stop eating or continue. im so stressed that somethings wrong with me. should i just be honest and tell her the next time I see her? i just can’t seem to open up to anyone about my eating disorder.
The Stickman Hook goal is to reach the finish line of each level by skillfully maneuvering around obstacles, avoiding hazards, and maintaining momentum.
Are you in search of an exciting game to unwind after a long day? tag game is the perfect option! Dive into a fun-filled adventure where you chase and tag your friends, enhancing your skills and unlocking cool features along the way. With vibrant graphics and engaging gameplay, this game promises a thrilling entertainment experience. Give it a try today and let us know what you think
In waffle game, every letter matters; only one letter swap will enable you to complete an unexpected word!
The best blog ever is your post. Your post is interesting and interesting io games
That’s a nice find bloodmoney game
Basketball Random is an exciting online sports game where players can participate in random basketball matches.