Birth control and reproductive health can be fragile ground. These posts are not meant to be a sociopolitical or religious conversation, or a position on women’s rights or feminism, nor am I trying to tell you what to do with your own reproductive health. My goal is to simply educate. It’s your right to know all your options so you can make a decision that is right for YOU.

Cervical fluid (CF) is something all women have, but nobody really talks about. So here we are, talking about it. Because it’s really important and can give you so much information about your reproductive health. If you’re currently on hormonal birth control for any reason, tracking your cervical mucus won’t give you reliable information because generally speaking, most birth control methods completely prevent ovulation. But, I think this info is still extremely helpful. At some point in your life you’ll probably come off birth control for one reason or another and having this info tucked away can be extremely empowering.
Monitoring your CF is not just for women trying to conceive. It’s also for women wanting to prevent pregnancy, women wanting to figure out an issue with their cycle, and really anyone looking to learn more about their body and reproductive health. Most of us, or at least myself, go through our teens and twenties knowing none of this information. My goal is simply to get it out there, to start the conversation, keep the conversation going and to be a resource. Take the parts of this post that feel helpful for you, and leave the parts that don’t. You are the one ultimately in charge of your health and you get to make decisions that are best for you. My hope is to provide as much information as I can so you can make the most informed decision that you can about your reproductive health.
So what is cervical fluid?
That mucus-y like fluid in your underwear or on the toilet paper when you wipe that kind of looks like snot and comes and goes, sometimes changing in consistency and appearance…..that’s your cervical fluid. For many women, it’s gross and shameful and something we don’t talk about. A lot of women are confused by this stuff, but it actually serves an incredible purpose and can tell you so much about your fertility and reproductive health. Men have seminal fluid and women have cervical fluid. As a whole, it seems men carry zero shame around their fluid. Women shouldn’t either.
Cervical fluid does a few key things. It protects sperm from the acidic environment of the vagina, it provides nutrients to sperm and it’s how sperm get through the vagina and to the egg for fertilization – the sperm can’t really swim without it.
After your period ends, estrogen begins to rise as you approach ovulation. Cervical fluid is under the influence of estrogen. So as estrogen increases, your cervical fluid changes. The higher the estrogen, the wetter and more abundant your fluid is going to be.
Types of cervical fluid
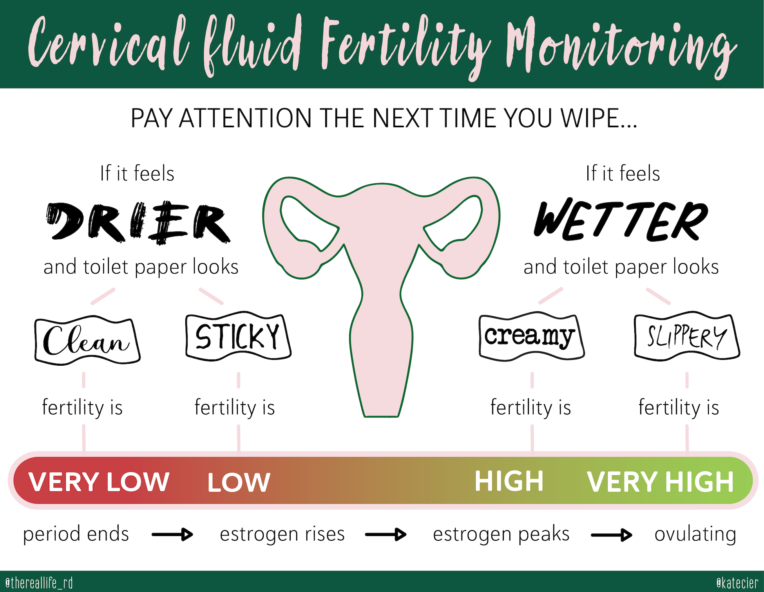
Although every woman has her own unique pattern, the typical progression is: dry —> sticky —> creamy —> wet & slippery right before you release an egg and ovulation takes place. Then after ovulation, cervical fluid dries up again until after your period.
It’s helpful to check your cervical fluid a few times a day. Next time you go to the bathroom and wipe, take a look at the tissue before tossing it into the toilet. You can also use your fingers to check…whichever way you prefer. You do you. Cervical fluid tends to pool at the opening of the vagina so you could do a kegel in order to move it down or simply insert your finger to get some…either one can be helpful so you don’t mistake a dry day for one that actually involved fluid.
Dry
If it feels dry to wipe and you see nothing – then you’re dry. This typically happens during the days following the end of menstruation before estrogen begins to kick back in. Dry means your fertility is very, very low. These would be considered “safe” days to have unprotected sex if you were trying to avoid pregnancy. ***While helpful for knowing when you’re fertile and not fertile, remember you need to use a barrier method (like condoms) to protect against STIs.
Sticky
If it feels dry to wipe, but you see sticky or crumbly white stuff in your underwear (or on the tissue) – it can actually look like dried rubber cement. The main thing to remember with this type, is that you see something in your underwear or fingers or tissue, but it’s not really wet. This is sticky CF. Estrogen is just beginning to rise. Your fertility is low.
Creamy
If it feels smooth when you wipe and you see a creamy, yellowish white, opaque looking fluid – almost like lotion – you have creamy CF. This type of fluid can stretch, but it doesn’t stretch far and will eventually break. This is the CF you will notice in the days leading up to ovulation as estrogen reaches its peak. You’re not the most fertile, but your fertility is high.
Fertile/Egg White
If it feels slippery, almost like the tissue is gliding when you wipe – this is super fertile, “egg white” cervical fluid. It’s clear or cloudy, wet, sometimes shiny and literally…looks like a raw egg white. If you put it between your fingers it would stretch at least an inch or more without breaking. Sometimes you can actually see it DRIP into the toilet (especially after a bowel movement) and almost form a small ball of mucus. Yep, we are going there right now.
This type of CF can also be super wet, almost like water. So if you don’t actually see anything, but feel really wet (almost like you’re leaking a small amount of urine during the day) that could be this type of CF. If you want to get pregnant, you’ll want to go have sex asap. Sperm can also live in ideal CF for up to 5 days, so even if you’ve had sex prior to actually ovulating (the egg survives for up to 24 hrs) you could still conceive if the sperm survive and go on to fertilize the egg. If you don’t want to conceive, use a barrier method (like condoms) or don’t have sex. This fluid means you’re very, very fertile.
Keep in mind if you’ve recently had sex, it can be easy to confuse seminal fluid with cervical fluid. First, if you remember, try to pee with some extra force after having sex so you can pee out as much of the seminal fluid as possible. Then when you pee again, kegal a few times as you pee. That should help flush out as much of the semen as possible. If you’re trying to get pregnant, don’t do this of course!
To be sure you’re not confusing seminal fluid with cervical fluid remember: seminal fluid is usually thinner and will evaporate, whereas cervical fluid won’t evaporate and is more viscous.
What if I don’t have regular cycles?
Monitoring your cervical fluid gives you the most insight into your reproductive health when you’re also tracking your basal body temperature, charting on some sort of calendar when your period starts and stops and even checking your cervical position. Temp and day of the month are objective measures that help you interpret the subjective signs of CF and cervical position.
If you have irregular or absent periods due to PCOS, hypothalamic amenorrhea (HA), endometriosis, breastfeeding, or other reasons, you can still monitor your CF (ideally with the other methods noted above) to get a sense of what your body is doing, but it wouldn’t be a reliable form of contraception. If you’re continually dry with no present CF, your estrogen levels are likely very low. If you see some sticky and/or creamy days, but in an irregular pattern then you know estrogen is shifting upward to some extent. While ovulation might be unpredictable or not happening at all, noting your CF “pattern” even if it’s an irregular pattern can still give you insight.
Essentially, your body needs to pass a certain estrogen threshold in order to ovulate. Once your body gets over that hump, LH (luteinizing hormone) surges and the eggs bursts out of the follicle and you ovulate. So for example, if you have HA or are breastfeeding and not getting a period at all, increasing wetness of your CF even if you aren’t ovulating yet could signal that estrogen is increasing and your body is “gearing up” to start ovulating again. Additionally, if you experience irregular periods for other reasons, monitoring your CF can let you know when you do actually ovulate – like with PCOS when women sometimes have longer, irregular cycles. Monitoring your CF can also let you know that you are having anovulatory periods, meaning you get your period, but you don’t ever see the fertile CF indicating you’ve ovulated in the ~2ish weeks prior to bleeding.
If you’re breastfeeding, recovering from HA or there’s another reason why you aren’t having a period at all, what can be helpful is to monitor your fluid for 2-3 weeks to get a baseline pattern. So for example, you might track for 3 weeks and notice you have fluctuating dry and sticky days. Or you have all dry days. Or you have all sticky days for those 2-3 weeks. That would be your baseline pattern. Then you can monitor for any changes in CF that stray from your baseline and that can indicate hormones are shifting and your body is working towards ovulation again.
What about coming off of birth control?
If you’ve recently come off birth control, your CF might be all sorts of irregular and confusing. If you were on birth control to manage symptoms like irregular cycles, heavy bleeding, cramping etc, those symptoms will likely return when you stop taking birth control. Some women resume ovulating right away after coming off – especially if you were on birth control solely for contraceptive purposes. For others it takes a little bit of time or a while depending on what kind of birth control you were on. I was prescribed birth control off and on for six years to “regulate” my cycle that was missing. In reality, I had hypothalamic amenorrhea so whenever I came off birth control, I never got a period. Birth control wasn’t fixing my problem. It was masking a serious issue. I needed to make drastic lifestyle changes in order to heal my body and give my reproductive system what it needed to function.
After coming off birth control, give it a few months and if your fluid doesn’t start resembling a regular pattern followed by a regular, monthly period I’d encourage you to go see your health care provider – depending on what kind of birth control you were taking, they should be able to give you insight into what you can expect with your period returning.
Other ways to monitor your fertility
I wrote a post about two years ago on fertility awareness methods here. If this topic is interesting to you, you can hop over there and read more about charting your temperature along with other methods. I don’t talk about checking cervical position in that post, but you can read more about that here.
I hope this post is informative and empowering. There is so much more to say on this topic! If you’re interested in learning more, this book is a wonderful resource. Cheers to not being ashamed of our fluids!

References
Owen M. (2013). Physiological signs of ovulation and fertility readily observable by women. The Linacre quarterly, 80(1), 17–23. doi:10.1179/0024363912Z.0000000005
Thijssen, A., Meier, A., Panis, K., & Ombelet, W. (2014). ‘Fertility Awareness-Based Methods’ and subfertility: a systematic review. Facts, views & vision in ObGyn, 6(3), 113–123.
Weschler, T. (2006). Taking charge of your fertility. New York, NY: HarperCollins.















Thank you so much for this, Robyn! I was definitely someone who had no idea “cervical fluid” was a term, and only heard the fluid described as “discharge”. I also felt pretty gross about it in my teens and early twenties, and even remember thinking in my teens that ANY discharge meant you had an infection. The only information I ever received about it was surrounding yeast infections and PID! It’s like we’re teaching girls “Here’s how to know if something is wrong”, but not “Here’s how to know that things are okay!”. Now I know what I’m looking at and it’s pretty cool to watch the CM consistency change over the course of each cycle.
that is a common misconception so you’re not alone – CF can be incredibly “healthy”, and it is most of the time!
Robyn,
Thank you for this information. Every time I read something you post about women’s health, it reminds me how incredible a woman’s body is. This information is important, and empowers women with more awareness about their bodies.
Thank you for this post!!
That is my hope – empowerment! Our bodies are AMAZING
I feel like this is the stuff missing from health class! I didn’t learn this until I was preparing to get married in the Catholic church, and took a class on NFP. I learned a ton about my body! Even people not needing NFP could benefit from this–it helps you know when you’re healthy, and when there’s something going on that needs to be looked into.
Agreed! I learned more about tampons lol
Thank you for this!
Question: Should a woman on BC have changes in cervical mucous? I always do and im nervous about that.
there could be fluctuations but you would not see a buildup from drier to wetter like you would if you were ovulating – but there are some types of bc (like the Mirena IUD) where ovulation is partially suppressed, although you’re still ovulating Mirena still works by preventing sperm from reaching the egg and thinning your uterine lining so it’s not conducive to implantation
I so appreciate that you cover things like this Robyn because I think a lot of women don’t know these things about their bodies. It’s so good to be able to understand my body better and not avoid these topics among our circles of women. <3 I love the way you explain it.
I’m so glad you’re enjoying this topic – I think it’s SO important. Thanks Emily!
Hello, Love your article! You are a true inspiration for us all! My Wife has got some amazing results with this new product. After having 3 kids she feels great and is a lot more happier. check it out. I’ll include the link below for anyone interested in losing some weight themselves.
https://bit.ly/2yNexXL
I know I am commenting on an older post but thank you for this information and content! I am a longtime reader and have a baby boy a few months older than Cal- starting to try for number two and this was a great refresher for me!
Thank you for presenting your ideas clearly and succinctly in this expertly composed text.
Your analysis of the problem is excellent! The reader is prompted to think by your compelling, cookie clicker and incisive arguments.
“Tracking cervical fluid is a great way to understand your reproductive health. Along with this, services like those at Balancemedspacan support overall wellness, from hormone balancing to body treatments, promoting a healthier you.”
Your presenting style is good, and I like your great ideas.
Cookingdom Game: Complete Walkthrough Guides
Your essential companion for mastering the Cookingdom game ✨ Access our detailed Cookingdom all Level Walkthrough Guides, simple cheats, and video walkthroughs.
Temple Blocks (also known as WoodenFish) is an online digital wooden fish platform that merges traditional wooden fish culture with modern technology. Users can tap a virtual wooden fish on desktop or mobile devices anytime, anywhere to experience immersive meditation and merit accumulation. The platform offers real‑time merit visualization and a global merit pool, designed to provide a simple, efficient, and enjoyable spiritual practice.
HentaiAI is an AI girlfriend interaction platform that allows users to engage with intelligent virtual girlfriends. Whether it’s sweet conversations, role-playing, or deep emotional connections, HentaiAI offers a unique companionship experience.
post but thank you for this information and content! I am a longtime reader and have a baby boy a few months older than Cal- starting to try for number two and this was a great refresher for me!
It’s so good to be able to understand my body better and not avoid these topics among our circles of women. <3 I love the way you explain it.
Free star symbols collection! Copy and paste Unicode star symbols instantly. Star text generator and aesthetic text tools for social media. ★☆
Browse complete star symbols collection. Classic stars, decorative stars, and Unicode characters. One-click copy to clipboard.
Interesting post on What Your Cervical Fluid Can Tell You About Your Reproductive Health; thanks for sharing it in a way that still feels grounded and readable. I’ve been testing Duct Tape AI for quick poster and mockup ideas lately, and posts like this are a nice reminder that clear presentation still matters most.