Adrenal fatigue is a term that has been circulating around the wellness world for years. It’s especially common in the realm of functional and integrative medicine. Perhaps you’ve heard of the term while browsing the internet or reading a book. Or maybe you were diagnosed by a healthcare professional with adrenal fatigue yourself. Some people say adrenal fatigue is a real diagnosis and some say it isn’t. So, is adrenal fatigue real? Is it an actual diagnosis that can be treated?

What is “adrenal fatigue?”
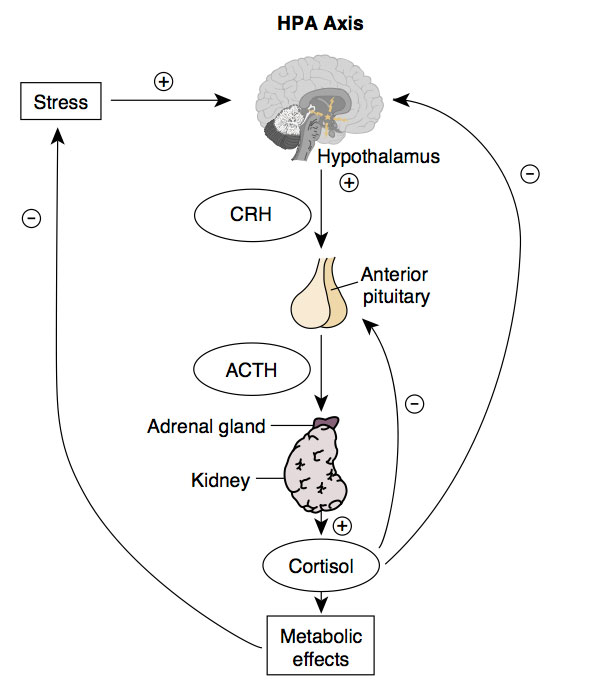
The adrenal glands are the last part of our hypothalamic pituitary adrenal (HPA) axis. Your HPA axis is responsible for your stress response aka your fight or flight response. (Here’s a 2 minute video explaining the HPA axis.) These two small glands sit on top of the kidneys and produce a variety of hormones. One of these hormones is cortisol. When our bodies experience stress, the adrenals produce and release small amounts of cortisol into the bloodstream. Cortisol does many things. It helps regulate blood sugar levels and metabolism, reduces inflammation, and regulates memory formation. In times of stress, cortisol increases heart rate, blood glucose, respiration and muscle tension. Cortisol also shuts down the body’s systems that aren’t necessary in times of crisis. We need cortisol to survive.
The term adrenal fatigue is used often in the media and by functional medicine clinicians to describe a condition in which someone experiences chronic, repeated exposure to stressful conditions. The repeated exposure of stress over time causes overstimulation of the adrenal glands. Eventually, the adrenal glands fail to function like they should.
What are the symptoms of “adrenal fatigue?”
The two most common symptoms associated with adrenal fatigue are tiredness and low energy. Other symptoms include brain fog, lack of motivation, depressed mood, and having trouble getting out of bed even after getting an adequate amount of sleep.
The problem is that fatigue and low energy are such general symptoms and many, many people go to their health care provider (HCP) with these symptoms seeking help. These generalized symptoms are associated with many medical problems, making it challenging to nail down a specific diagnosis. Anemia, autoimmune diseases, thyroid problems, mood disorders, problems with major organs, infections, sleep disorders, etc. are associated with low energy and fatigue.
When you go see your HCP, they get a thorough history, perform a physical exam and order diagnostic tests to help nail down a diagnoses. With general symptoms like fatigue, low energy, lack of motivation (symptoms associated with “adrenal fatigue”) the workup often isn’t helpful and lends few, if any, answers. Physical exam is normal. Blood work is normal. This can be perplexing and frustrating for you, the patient, but also the health care provider because there is no clear cut answer for the symptoms you’re experiencing. It can be really enticing to tell someone they have “adrenal fatigue” to explain their generalized symptoms of fatigue and low energy. Or maybe you’ve heard, “There’s nothing wrong with you.” or “It’s all in your head.” That can be really frustrating and invalidating as a patient too.
How is an adrenal fatigue diagnosis made and is it valid?
Practitioners diagnosing this phenomenon use a patient’s reported history and symptoms along with laboratory tests to make a diagnosis. This is problematic in many ways. These symptoms are so incredibly general. As far as the research goes, there is no validated symptom score to assess these symptoms. In contrast, the PHQ-9 and PHQ-2 are well researched and valid assessment tools used in primary care and mental health settings to evaluate mental health. There is no such tool for assessing adrenal fatigue. There are also lab tests used in naturopathic/functional medicine settings and tests marketed on the internet to detect adrenal fatigue. Unfortunately, there is no compelling data to validate these tests. The same goes for hormonal tests and food allergy tests marketed on the internet and used in these clinical settings. Just because a test is offered, doesn’t mean it’s valid.
I think it’s important to note that adrenal fatigue and adrenal insufficiency are not the same. Adrenal insufficiency is a well researched and legitimate medical condition that has defined symptoms and can be diagnosed with laboratory tests.
What the research says
There was a systematic review published in 2016 exploring the validity of adrenal fatigue. Systematic reviews are the cream of the crop when it comes to research. They give us the highest quality evidence. The review published included 58 studies and found no evidence for the diagnosis of adrenal fatigue. As of now, we have no formal criteria to define what adrenal fatigue is nor do we have criteria to diagnose adrenal fatigue. If you want to geek out, you can read the full review here.
The symptoms are real, adrenal fatigue is not
While it can be really frustrating to have these symptoms and be told it’s all in your head, know this: Your symptoms are real. What you feel is real. It’s just that adrenal fatigue is not a real diagnosis. Not having a biological explanation for symptoms can be frustrating, disappointing and emotionally draining. Mental health diagnoses like anxiety and depression can manifest symptoms similar to those associated with adrenal fatigue. Especially in today’s fast paced society, feeling anxious and/or depressed is not uncommon and you are not alone. Know that! If you feel like you are experiencing symptoms that are attributed to “adrenal fatigue” I’d encourage you to take a step back and do some reflecting. What are the stressors in your life? How is your sleep hygiene? How is your mental health? Your emotional health? Is the exercise you engage in helping you live a less stressful or more stressful life?

Recommendations to “treat” adrenal fatigue have the potential to do more harm than good
Although getting a diagnosis for a medical condition that doesn’t actually exist isn’t good medicine, it’s the recommendations to follow that have the potential to be quite harmful. If you google adrenal fatigue you will find pages and pages of information that I think actually cause more psychological distress and confusion.
If you’re feeling tired and stressed, the last thing you need is more things to do and fix. The recommendations for adrenal fatigue are cloaked in diet culture. The primary recommendation is to cut out a bunch of foods from your diet – to essentially go on an elimination diet. The nutrition prescription is to eliminate all processed foods, sugar, dairy, gluten and starchy carbs. Dieting is one of THE most stressful things to put your body through – emotionally, mentally and physically. There is also a slew of supplements to take and other alternative therapies to embark upon. I’m more stressed just typing that.
My concern is not only the lack of evidence to support these extreme recommendations. I also worry about the high potential for these “adrenal fatigue” treatment recommendations to perpetuate disordered eating habits and more stress. Of course, high levels of stress isn’t a good thing for our long term health. High levels of stress can, and likely will, negatively impact our health. Wrapping all of these general symptoms up into a illegitimate diagnosis and then “treating” the condition with elimination diets among other recommendations that have no scientific evidence is a problem. It’s oversimplifying a bigger problem and giving people a “protocol” to fix an issue that is far more complex. Controlling food does seem really enticing when other parts of your life feel out of control. Following guidelines and steps is really comforting when we feel overly stressed and aren’t sure where to go next.
What you can do instead
These recommendations aren’t black and white. They aren’t a protocol. If you sat these recommendations next to the “adrenal fatigue solution” book, you’d sell more copies of the “solution” because it’s far more appealing to people. Diets do sell. They just don’t work.
- Sit down and figure what you actually need to do in your life versus what you think you need to do.
- Prioritize your sleep – get at least 7-8 hours every night.
- Set boundaries in your life. What things are you saying yes to? That list should be incredibly small. Protect your yeses!
- Nourish your body with a variety of foods at regular intervals throughout the day. If you don’t eat 3 meals a day, start there. If you don’t get hunger cues, eating 3 meals and ~3 snacks a day (so you’re eating every 4ish hours) is a good place to start.
- Drink your morning coffee, but choose something other than caffeine after lunchtime. Caffeine later in the day can make it hard to fall and stay asleep. If you rely on coffee to “make it through the day” take a step back and figure out what you need to do in order to not rely on caffeine.
- Drink water! At least 64 oz. Sounds elementary, but there have been so many times when hydration has been the key to alleviating a symptom.
- Spend time with people that make you feel good. Surrounding yourself with people who add to your life (not take away) can move mountains when it comes to our mental and emotional health.
- Re-evaluate your exercise routine. Do you use exercise as punishment? Is exercise something you feel obligated to do or something you view as a “should do?” Are you exhausted before or after working out? If any of these resonate, I’d really encourage you to take a step back from intentional exercise. Walk. Play with your kids or your dog. Do some relaxing yoga. Here’s a post on healing your relationship with exercise.
- Start a mindfulness practice. That might sound woo-woo, I get it. I don’t resonate with the word “mindfulness” as much as I do “chill out.” Stretch on the floor for 10 minutes before bed, take a morning stroll without your phone, or deep breath for 60 seconds.
- Unplug from devices and screens. Technology is awesome, but it can also clutter our brains because it keeps us constantly stimulated.
Final Thoughts
Stress is real. It certainly affects our health. Your symptoms are also real. Although the above list is not exhaustive and everyone’s journey will be different, I hope this post and these tips give you a starting point. Remember, slow baby steps. Change in and of itself is stressful. Start with one change and implement it over the course of a week or two. When you’re ready, move on to something else that feels manageable. Over time, all these small changes will help you live a healthier, happier and more authentic life that aligns with your values.
If you’d like, you can sign up here for my free mini email course on healing hormones – it gives you some starting points and practical steps so you feel your best physically, mentally and emotionally.
















I was experiencing these symptoms after the birth of my second child, along with a sporadic menstrual cycle. I was given an internal ultrasound which showed very cystic ovaries. My doctor ordered bloodwork, anticipating a PCOS diagnosis but instead my results came back showing frighteningly low levels of DHEA and testosterone. I saw countless specialists, including an endocrinologist, and was ultimately given a “diagnosis” of adrenal fatigue. The whole process was frustrating and did not sit well with me – not one doctor talked to me about my stress level or lifestyle. I slowly made some of the changes you suggested here and am hoping for some better bloodwork results in the future! Thanks for all you do.
I’m so sorry you had these frustrations Whitney! I know it can feel really frustrating to not feel heard or truly cared for. Wishing you all the best in caring for yourself!
I really appreciate this post. I like that you said the symptoms and feelings are real, but an adrenal fatigue diagnosis is not. Part of the reason I’ve stepped WAY back from the wellness community on social media is because i felt like so many people were trying to label their stress, anxiety, and tiredness as an illness. As someone with an actual chronic disesase (type 1 diabetes) I got really frustrated watching people making themselves think they were sick. In a way, it seems like a cop out to label the life stress that we all have some control of as “adrenal fatigue.” It’s like instead of doing the hard work of making some of the changes you highlighted at the end of the post, people just want to have a reason to take exotic supplements and eliminate food groups. This might be sounding more bitter than i intend, but it’s so clear to me that we all need to return to basics and uncomplicate our health and also take some of the focus away from it… these symptoms are not ideal, but they are also very HUMAN- espeically, like you said, in this crazy digital age we live in. I personally have found such a dramatic improvement in my mental AND physical health from deleting instagram from my phone. I finally have the space to feel my OWN feelings and be in touch with my own body instead of having a bunch of wellness influencers in my head, literally influencing what i think I need/how I think I am feeling. It’s crazy how that one simple change has elevated my entire existence.
Yes yes yes!
“It’s like instead of doing the hard work of making some of the changes you highlighted at the end of the post, people just want to have a reason to take exotic supplements and eliminate food groups.”
I think that “wellness culture” can certainly be cloaked in a lot of pseudo science and made up diagnoses that then come with poorly researched, diet culture stained, “treatments”
Hi Robyn! Thank you so much for this post and your blog in general, I really love reading all of your posts! I was just wondering if along with these symptoms of “adrenal fatigue” like tiredness, etc, would elevated blood sugar be a symptom as well? I know cortisol and the adrenals are involved with metabolism, etc. Thanks!
Stress and lack of sleep can certainly cause blood sugar issues!
Just saw this! Thank you so much :)!
Thank you for this. I know many people who get swept up in the claims of functional medicine people. I hate that certain individuals in positions of authority either do not do their research or intentionally make people feel bad about themselves to sell things. I appreciate your balanced approach to health!
Have that voice of “authority” is something the health profession cannot take lightly – people look to health care providers and put their trust in them so we MUST deliver evidence based and ethical care. Thanks for sharing!
Excellent post, Robyn. So well explained, while also being compassionate towards people experiencing these symptoms. And the concrete list of things to do to help at the end of the post – amazing. I’m going to use this article as a reference for patients who come to me with this “diagnosis.”
So glad you found it helpful! The symptoms certainly are real and validating one’s experience I think is so important as clinicians. Thanks for using this as a resource for patients!
I love the way you uncomplicate things, Robyn. I’ve realized that really IS the key to health, just keep it simple. Eat intuitively, get sleep, drink water. We don’t need to be downing collagen or overdosing on matcha or putting butter in our coffee, or taking 47 vitamins a day, or ANY of the other weird health trends that have popped up lately. It’s all in support of an industry that doesn’t care about us, they care about making $$ and that’s the truth.
Thank you, Robyn!
🙌🏼🙌🏼🙌🏼
We tend to go to the extremes with caring for our health – if you don’t have a medical diagnosis, health doesn’t have to be fussy, expensive or complicated. That can LEAD to health problems! Yes, the wellness industry at the end of the day is a business
Thank you Robyn! Would love your perspective on other “diagnosis” non-celiac gluten sensitivity, lactose intolerance, fructose intolerance, food intolerance/sensitivities, leaky gut. I come across so many of these when working with ED patients, and some of them are diagnosis given by medical professionals. I recently had a patient following a gluten free diet due to a dermatologists diagnosis of gluten sensitivity. I had another patient avoiding major food groups after receiving an iga antibody test which said she was “allergic” to major food groups – after actual allergy testing it was found that she doesn’t have any food allergies. Our current diet/wellness culture creates so much food fear and its hard to get patients to see this when other medical professionals are involved. Thank you for all you do!!
food sensitivity tests are quite problematic…this is certainly a very important topic! I’d encourage you to listen/read Marci Evans work – she knows quite a bit about GI stuff and EDs. The gut is fragile and compromised in the presence of an ED so of course there is going to be GI symptoms…that doesn’t mean the food is the cause. The picture is much more complex! I wrote a post on this as well.
https://www.thereallife-rd.com/2017/07/eating-disorder-gastrointestinal-issues/
This post is so timely. I just listened to a podcast which spoke to this from an integrative medical doctor. It threw me a bit because the podcast is hosted by an IE based person who has been in recovery from an ED for several years. It made me question things again and I felt a little off kilter – helps so much to be grounded again from your post! Thank you Robyn!
Glad this post felt grounding Suzanne! Unfortunately there are a lot of people out who have an inaccurate definition of IE. Not saying this person who was hosting does, but something to be watchful of as you consume content 🙂
This is so helpful; I’ve seen a lot of people talk about adrenal fatigue, but this helps in that I think it’s often people just wearing themselves out in our busy culture; your reminder to check in and slow down, sleep, nourish, and do all the things that are so important is so good.
keep it simple! 🙂
This was so great Robyn. Thanks for sharing this.
you’re so welcome Tracy!
This is such a wonderful post, Robyn ❤️🙏. I’ve dealt with infertility and have been in and out of doctors offices for the past years trying to figure out what in the world is going on with my body. So many ‘general’ symptoms that no one practitioner can seem to figure out. I just recently have come to the point of wanting to take a break from it all. And instead of trying to find a solution and a fix for it, just want to focus on nourishing myself with things that feel good. Your post is such a wonderful reminder of that… to tap into my intuition for the things that bring me happiness and calm. That goes a long way. ❤️
My heart goes out to you so much in your fertility journey Valerie <3
Take a step back, rest, be gentle with yourself - I think learning into your intuition is a good thing too. Thinking of you!!
SO helpful! I find so much comfort in your posts like these!
Amazing post and these sentences really resonated with me: “Controlling food does seem really enticing when other parts of your life feel out of control. Following guidelines and steps is really comforting when we feel overly stressed and aren’t sure where to go next.” It’s super easy to get frustrated with friends, family and clients who are following the latest fad diet but when you think about it from this perspective, I can totally see why this happens.